
While COPD is usually characterized as a breathing disorder, it is a complex disease that can cause a variety of different ailments besides respiratory decline. One of of these is back pain, a serious ailment that afflicts nearly fifty percent of patients with COPD
Back pain caused by COPD can be mild or severe, and in extreme cases even debilitating. It can be acute and short-term, or it can be chronic, lasting for days or months at a time.
Besides being plain painful, back pain can interfere with your daily life and make it difficult to continue your normal routine. If severe, it can even interfere with your COPD treatment and leave you unable to exercise and do other things that are important for your health.

Luckily, back pain is very treatable, and there are many simple things you can do in your daily life to minimize your back pain. In this guide, we're going to introduce you to a variety of natural techniques and practical methods you can use to get relief.
Whether it's acute or chronic, most types of back pain can be reduced with healthy habits and lifestyle changes like exercise, posture, and diet. That's why it's so important to examine your everyday habits and lifestyle to identify things that might be contributing to your pain.
If you don't start treating your back pain now, it may only get worse over time. That's why it's important to take action now, before the pain takes an even greater toll on your life and your ability to manage your COPD.
Instead of waiting it out or assuming your back pain will go away on its own, learn what kinds of actions you can take in your daily life keep your back healthy and strong. In this article, we are going to help you do just that, by helping you understand why COPD causes back pain and how you can use a variety of simple methods to treat your back pain at its source.
Understanding Back Pain and COPD

Back pain is a very general symptom that can have a variety of different causes. But if you have COPD, your back pain could be directly or indirectly caused by your disease.
COPD-related back pain tends to be chronic and also tends to affect the lower back. In fact, research shows that more than forty percent of people with COPD experience chronic lower back pain.
COPD patients can suffer from any type of back pain or a combination of multiple kinds at once. Here is a quick overview of the main types of back pain and how to recognize them.
Acute Back Pain

Acute back pain is usually defined as short-term back pain lasting for less than six weeks. It is usually caused by injury or trauma and resolves relatively quickly.
Many people feel acute back pain as a sharp pain or dull ache. The pain can be minor or it can be severe enough to affect your daily life, making it difficult to move, work, and sleep.
Chronic Back Pain
Chronic back pain is back pain that lasts longer than six weeks and doesn't get better on its own. It can be caused by inflammation, strain, or injury and doesn't usually get better on its own.
Chronic back pain is often in the lower back and feels like a deep aching or burning. It tends to travel from your back to your hips and legs and get worse when you stay still for long periods of time.
Mechanical Back Pain
Mechanical back pain is any kind of back pain caused by a mechanical injury to your muscles or spine. That includes pain from strain, accidental injuries, poor posture, and other physical causes.
Inflammatory Back Pain

Inflammatory back pain is, in a way, more chemical than it is physical. It is caused inflammation inside your body that damages the tissue of your muscles, bones, and/or joints in your back.
Back pain caused by inflammation is often chronic and gets worse when you sit for too long or don't get enough physical activity. Chronic back pain is usually more difficult to relieve and manage than acute or mechanical back pain, and the most common treatments are exercise and anti-inflammatory drugs.
How COPD Causes Back Pain
Osteoporosis
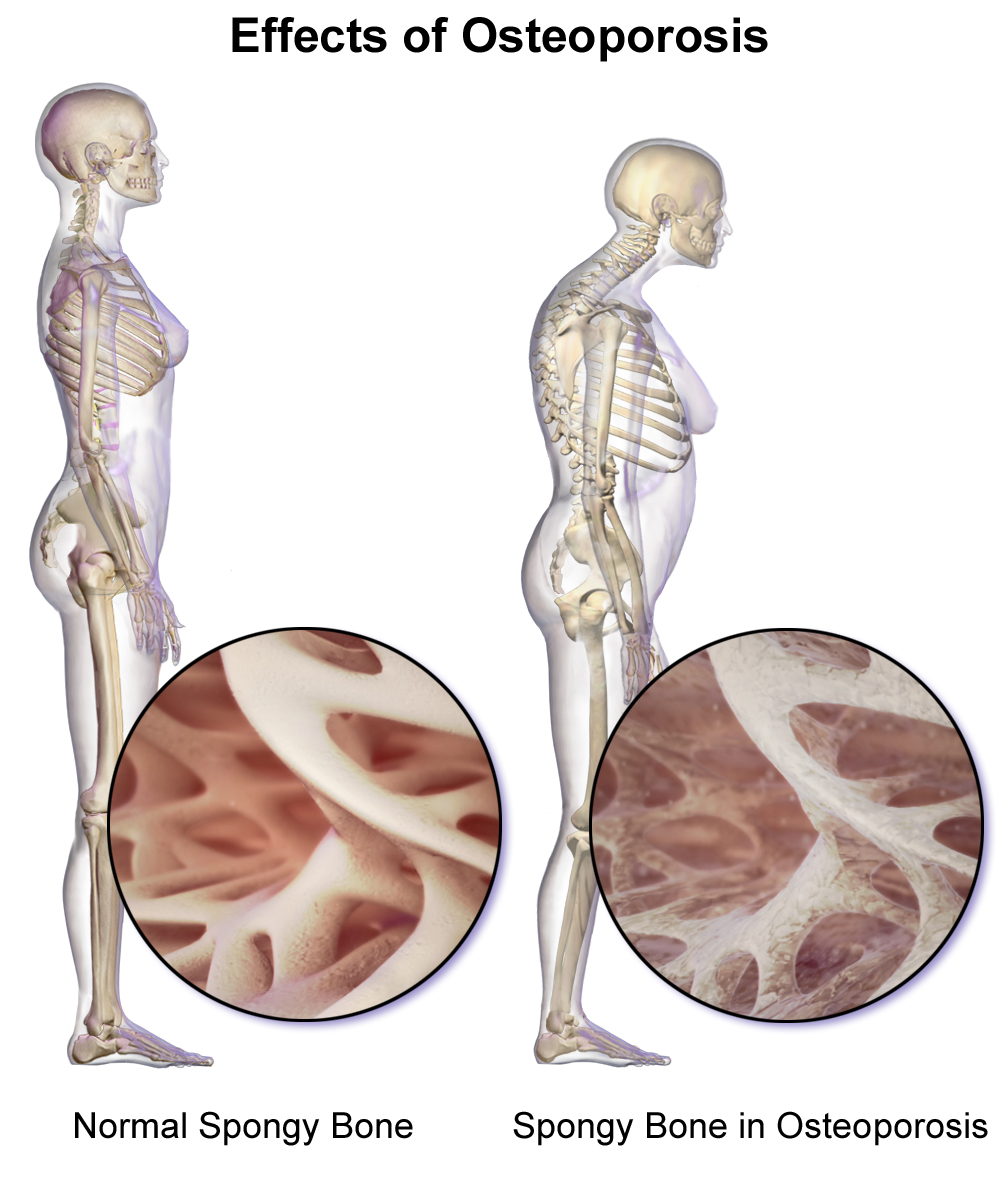
Osteoporosis is a common cause of back pain in people with COPD. You can get osteoporis if you don't eat enough calcium, which impairs your body's ability to build and repair your bones.
As a result, your bones become very thin, weak, and brittle. They can become so weak, in fact, that a minor bump, fall, or even normal activities and movements can cause your bones to break.
Most people don't notice any symptoms in the early stages, but osteoporosis can cause severe pain as it progresses and causes invisible injuries. This pain usually stems from tiny cracks, breaks, and compression fractures that patients often don't even realize they have.
The most common causes of osteoporosis-related back pain are spinal compression fractures, which usually cause a more severe kind of back pain. This type of injury tends to hurt most when you stand, walk, twist, and bend, and tends to lessen when you lie down.
Osteoporosis is particularly common in COPD patients, who often struggle to get enough nutrients from their diet—including calcium—because of how the disease affects their bodies. COPD patients also tend to avoid exercise, which weakens your bones and can lead to bone-related back pain.
Lack of Physical Activity (Muscle Atrophy and Disuse Syndrome)
Not getting enough exercise is another major factor that makes people with COPD more prone to back pain. This is a risk for patients with advanced COPD, in particular, who often find it difficult to stay active because of their severe physical and respiratory symptoms.
Not getting enough physical activity causes your muscles to break down (atrophy) and can even weaken your bones and joints. It also hurts the flexibility of your back, which can cause stiffness and pain when you move.
Unfortunately, many people avoid exercise when they have back pain, which can end up making it even worse. This can start a vicious cycle where lack of physical activity causes back pain, and untreated back pain can causes patients to avoid physical acitivity even more.
Patients that live too sedentary a lifestyle can also develop disuse syndrome, a disorder that stems from not using your body enough. It can lead to back pain, other chronic pains, cardiovascular disease, and mental disorders like anxiety and depression.
Chronic Inflammation

One of the most direct ways that COPD can cause back pain is through chronic inflammation. This happens when your immune system's inflammatory response stays active all the time, which is a very common symptom of COPD.
Chronic inflammation wears down your body and can cause a variety of serious health conditions, including heart disease and depression. Another side effect of chronic inflammation is chronic pain, including chronic back pain, which you may feel in your muscles, bones, and joints.
Inflammatory back pain is different from mechanical back pain, and can be a sign of arthritis. While mechanical back pain usually comes from physical injury to the muscles and bones in your back, inflammatory back pain is the result of inflammation in the joints of your spine.
Back pain caused by inflammation lasts for at least three weeks and is usually felt most in the lower back. In severe cases, it can lead to a type of arthritis called ankylosing spondylitis, which can affect a variety of joints in your body, and can even cause sections of your spine to fuse together in its later stages.
Inflammatory back pain gets worse when you don't move around for long periods of time and improves with movement and exercise. It doesn't get better with rest and tends to be more severe in the morning after you've been lying in bed all night.
How to Treat Back Pain from COPD
If you have COPD and suffer from back pain, you don't have to suffer in silence. There are many different options for treating back pain, including home treatment, medication, and implementing new habits in your daily life that support a healthy back.
Practice Good Posture

Bad posture can both cause back pain and make existing back pain worse. It can cause muscle strain and stiffness, compress your bones and joints, and lead to variety of back aches and pains.
On the other hand, good posture supports your spine and the muscles in your back so they don't get tired or strained. By adjusting your posture, you can relieve existing back pains and prevent more pain in the future.
People with COPD are particularly prone to bad posture because of their respiratory symptoms and tendency to avoid exercise. Because of this, it is particularly important for you to watch your posture if you suffer from COPD.
Sleeping posture, in particular, is a problem for many people with COPD. One reason for this is that lying down on your back puts extra weight on your chest, which makes it more difficult to breathe.
One solution to this is to sleep on your side, which many patients find makes it easier to breathe and sleep at night. However, to keep your spine aligned and prevent back pain, you should also put a small pillow between your knees.
Another common posture issue among people with COPD is bending over at the waist whenever they feel short of breath, because they feel it makes it easier to breathe. However, you can breathe just as well and prevent unnecessary back pain by practicing breathing exercises in an upright posture.
If you suffer from back pain and COPD, don't underestimate the power of good posture to improve how you feel. Changing your posture habits can not only relieve your back pain, but it can improve a variety of other symptoms of COPD.
To learn more about how your posture can affect your COPD, visit our guide on how to improve your COPD with good posture.

Here are some more tips for practicing proper posture to reduce back pain with COPD:
Good Standing Posture:
- Stand completely upright with your shoulders parallel to your hips and feet.
- Bend your knees slightly and place your feet slightly apart at about shoulder's width.
- Keep your shoulders pulled back, yet relaxed. Do not let them slump forward.
- Keep your chin parallel to the ground.
- Put your weight on the balls of your feet and shift from one foot to another if needed.
Good Sleeping Posture
- Sleep with a good-quality, firm mattress and pillow.
- Sleep on your back or on your side, but avoid sleeping on your stomach.
- If you sleep on your back, put a small pillow under your knees to help keep your spine straight.
- If you sleep on your side, put a small pillow between your knees to keep your hips and spine aligned.
- Consider getting a special pillow or mattress designed to aid with good sleep posture or back pain.
Don't Stay Sedentary

Many cases of back pain are caused by lack of physical activity, which is something that people with COPD often struggle with. Exercising with COPD symptoms can be very challenging, and too many patients simply give up and settle into an unhealthy, sedentary lifestyle.
However, being inactive leads to even more problems, including back pain, disuse syndrome, and worsened COPD symptoms. The more sedentary you are, the worse your symptoms will get, and the more your aches and pains will multiply.
This happens because, when you don't get enough exercise, your muscles atrophy and get weaker and stiffer; this can lead to both long-term and short-term back pains. Additionally, as your back muscles lose strength and tone, they also become more prone to cramping and injury.
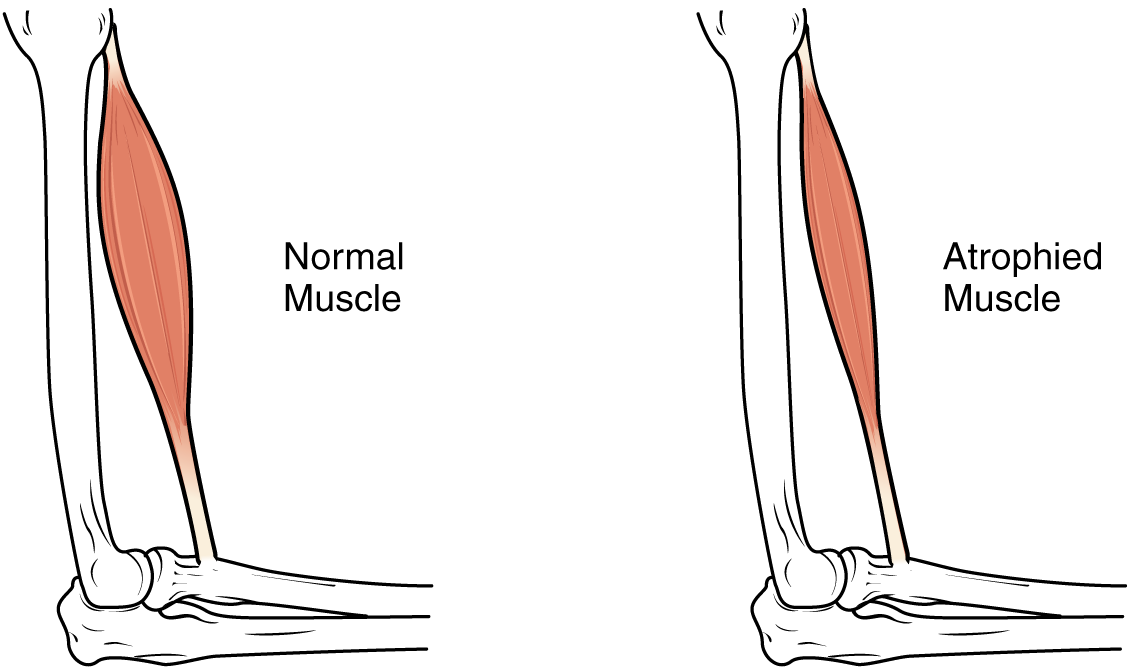
The solution to this is getting more physical activity and doing exercises that limber up and strengthen the muscles in your back. Regular exercise will not only protect your back from injury, but it can even relieve your back pain significantly.
Regular activity is especially helpful for your back if you live a sedentary lifestyle or suffer from inflammatory back pain. In those cases, getting more movement and exercise is perhaps the single most effective thing you can do to reduce your pain.
In order to keep your back in good shape, make sure to get at least 20 minutes of moderate physical activity at least three times per week. It also helps to get up at regular intervals throughout the day to stretch your back, shoulders, and spine.
Exercise Your Back

Many different kinds of physical activities can relieve pain and pressure in your back. Anything that gets your body moving can help, including stretching exercises, strength training, and cardiovascular activities like walking or biking.
Stretching and strength training exercises are particularly helpful for loosening up your back muscles and strengthening the muscles that help support your back. Muscle groups to target include your abdominal muscles, hamstring muscles, and the muscles in your upper and lower back.
For the best results, you should do strength training exercises at least four times a week in sets of 3-5 repetitions. It may take some time to see results, but you should notice an increase in strength and a decrease in pain within about six weeks of starting exercise.
It is normal to feel some pain and discomfort when you first start working out and strengthening your back. However, you should be careful to start small, take it slow, and stop if it makes your pain worse.
It helps to start out with low-impact exercises like walking, stretching, and water aerobics that won't over-stress injured muscles and joints. Abdominal muscle exercises are another great place to start because they are simple to do and they help support your back.

Depending on the severity of your pain, you may need to work with a physical therapist that can help you more gradually step up your activity and condition your back. You can also ask your doctor to help you put together an exercise plan that considers your limitations from back pain and COPD.
Along with regular physical activity, exercises that stretch and tone important back-supporting muscles can relieve pain and strengthen your back against future injuries and strain. To learn more about specific exercises you can do to target back pain, take a look at some of the following online resources.
Here are some great resources for learning exercises that strengthen the muscles supporting your back:
- 10 Exercises to stretch and strengthen your back (with helpful images to demonstrate) from the Mayfield Clinic
- 5 Exercises to relieve lower back pain (with helpful images to demonstrate) from the National Health Service
- 4 Simple exercises to strengthen your spine from the Spine Health Institute
- 3 Strength training exercises for your back muscles from SpineHealth.com
- 3 Strength training exercises for your abdominal muscles from SpineHealth.com
Always Ask Your Doctor Before Increasing Exercise
It's important to understand that not all types of back pain can be improved with exercise; in fact, you could make certain types of back pain worse by moving around. That's why you should always see your doctor and get your back pain diagnosed before starting any new exercises or treatments.
If you experience back pain in the form of stiffness, cramping, tightness, or sharp, shooting pains when you move around, then it may be a sign that your back muscles need more exercise and tone. However, very severe pain could be a sign of another type of injury that you could make worse by increasing your activity.
If inactivity contributes to your back pain, then making an effort to live a more active lifestyle could significantly relieve your pain. However, you should always get your pain evaluated by a medical professional before making any major changes to your level of activity.
Eat Enough Calcium and Vitamin D to Prevent Osteoporosis

Osteoporosis is a debilitating disease that can cause severe back pain and lack of physical mobility over time. It is also irreversible; once you've lost bone density from osteoporosis, there's nothing you can do to get it back.
The good news is that osteoporosis is almost entirely preventable, since it is almost exclusively caused by calcium deficiency. All you have to do is get enough calcium and Vitamin D in your diet to prevent yourself from ever developing this disfiguring disease.
That's why the best way to prevent osteoporosis-related back pain is to make sure you get enough calcium every day from the different foods that you eat. If you struggle to eat a balanced diet or suffer from vitamin deficiencies, you may need to take a calcium supplement too.
It's also important to get enough Vitamin D, which your body needs to help it absorb the calcium you eat. Having a vitamin D deficiency can cause a calcium deficiency, which in turn causes osteoporosis.
According to US dietary guidelines, most people should get about 1,000 milligrams of calcium per day, or about two servings of calcium-rich foods. However, older adults need more; if you are a woman over the age of 50 or a man over the age of 70, you should increase your calcium intake to about 1,200 milligrams per day.
US guidelines recommend that all adults get at least 15 micrograms of vitamin D every day, or at least 20 micrograms for adults over the age of 70. You can get your daily amount from vitamin D-rich foods in your diet and from the sun, which causes your body to synthesize Vitamin D when sunlight touches your skin.

Unfortunately, both calcium deficiencies and vitamin D deficiencies are very common in the United States. If you suspect that you don't get enough of either of these vitamins from your diet, you may need to start taking a daily supplement. However, it's a good idea to see your doctor first to check for a deficiency.
Here are some foods you can eat to get more calcium in your diet:
- Soybeans
- White Beans
- Collard Greens
- Kale
- Spinach
- Calcium-rich fish (e.g. salmon, sardines, and rainbow trout)
- Calcium-fortified foods (e.g. some orange juices, cereals, and grains)
Here are some rich sources of vitamin-D that can help ensure your body absorbs enough calcium:
- Beef liver
- Egg yolks
- Cod liver oil
- Fatty fish (e.g. tuna, salmon, mackerel)
- Vitamin D-fortified dairy products (e.g. cheese, milk, and soy milk)
- Vitamin D-fortified orange juice and cereals
- Sunlight (About 10-20 minutes of direct sunlight during the middle of the day should meet your daily requirements. However, it may take longer during the winter, if you go out in less intense sunlight, if you have dark pigmented skin, or you don't enough skin exposed to the sun)
Apply Ice and Heat

Heat and ice are the classic treatments for pain in your muscles and joints. It's particularly helpful for pain caused by swelling, inflammation, and stiffness caused by injury or arthritis.
Because of this, heat and ice are often recommended as a treatment for chronic and acute back pain. Ice helps by reducing inflammation and numbing the general area, while heat helps by increasing blood flow to the area and promoting healing and flexibility.
If you experience back pain from an acute injury like muscle strain or soreness from exercising, you should ice the area for the first one to three days. Once the swelling and inflammation recedes, apply heat to the area to stimulate blood flow and healing.
For chronic back pain, the benefits of heat and ice are less clear. Some patients experience symptom relief from heat, ice, or both, but others don't experience any reduction in pain.
If you suffer from chronic back pain because of your COPD, then you can try applying heat or ice to the painful area to see if it relieves any pain. You might also try applying heat to your back before exercising, which some patients find can improve their flexibility during exercise and reduce muscle sorness afterward.
Watch Out for Acid Reflux

Researchers have found that people with COPD are more likely to experience both lower back pain and gastroesophageal reflux disease (GERD). GERD is a disorder that causes your stomach acid to leak out of your stomach and into your esophagus, causing sore throat, heartburn, and other painful symptoms.
GERD can also cause “referred pain,” which describes the phenomenon of experiencing pain in a different spot than where the pain originates from. This happens when the nerves in one part of the body (e.g. your stomach) are closely connected with nerves in another part of the body (e.g. your back).
As a result, whenever you experience pain in one area, it can cause you to feel pain in the other area, too. In the case of GERD, many people experience referred lower back pain because the pain of acid reflux gets referred to the muscles in their lower back.
If you have COPD and experience lower back pain, then it might be worth considering acid reflux as a potential cause. You should at least know how to recognize the signs of GERD and talk to your doctor if you notice any symptoms.
Acid reflux is a common disorder, and it seems to be particularly common in older adults and people with COPD. It can also be worsened by tobacco smoking, which is a problem for the majority of people with COPD who smoke or have a history of smoking.
Usually, the best way to treat GERD is to change your diet and eating habits. Things like eating smaller meals and avoiding acidic foods can go a long way toward reducing GERD symptoms and chronic lower back pain.
Here are the main symptoms of GERD to watch out for:
- Acid reflux (regurgitating sour liquid or bile, especially when reclined)
- Lower back pain (especially if it appears after eating)
- Worsened COPD symptoms when lying down
- Difficulty sleeping at night
- Burning chest pain or heartburn (especially after eating)
- Sore throat (especially in the morning after you wake up)
- Difficulty swallowing
- Chronic cough
Here are some tips for managing GERD to reduce your lower back pain:
- Avoid tobacco and alcohol
- Avoid acidic drinks like coffee, soda, caffeinated beverages, and black tea
- Avoid acidic foods (e.g. citrus fruits, tomatoes, etc.)
- Avoid fried foods and fatty foods
- Avoid minty foods (e.g. peppermint and spearmint candies and gum)
- Avoid fatty dairy foods and milk (opt for low-fat versions instead)
- Avoid eating before bedtime and don't lie down after eating
- Avoid wearing clothes that feel tight around your chest, stomach, or waist
- Manage your weight and maintain a healthy BMI
- Limit how much food you eat at once; instead of large meals, eat several smaller meals spaced out througout the day
Try Massage Therapy
While the research on massage therapy for back pain is not conclusive, many researchers believe it can be an effective therapy for certain types of back pain. Studies show that massage may be able to improve lower back pain, upper back pain, and chronic back pain.
Massage therapy seems to be most effective at reducing pain in the short term, although some studies suggest the relieving effects of massage could last for several weeks or months. Researchers have not yet been able to determine which types of massage are the most effective, but studies have identified relaxation massage, structural massage, and thai massage as potentially helpful therapies.
Massage therapy can also help relieve muscle stiffness, making it easier to exercise and strengthen your back. It can also help you relax, release tension in your muscles, and possibly even reduce COPD symptoms.
In fact, early research suggests that massage therapy may even improve exercise endurance and reduce shortness of breath in patients with COPD. Because of this, massage is often recommended for its potential to improve a variety of ailments caused by COPD, including chronic back pain.
Try Physical Therapy
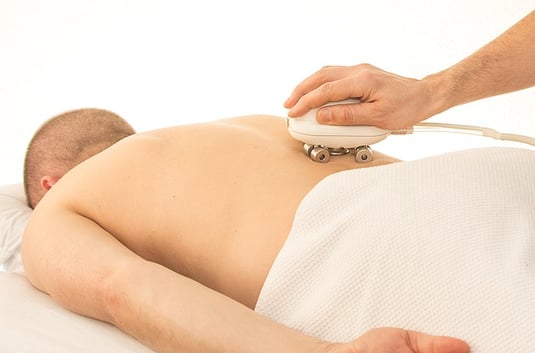
If you experience chronic back pain that lasts for more than a few weeks, you might benefit from physical therapy. However, you might need physical therapy even sooner if your doctor recommends it or if you are in severe pain.
Physical therapy can help you reduce your pain and improve your range of movement through gentle stretches and exercises. A physical therapist can even apply other therapies, such as ultrasound therapy and electrical nerve stimulators (TENS therapy), which may help relieve your back pain.
Another benefit of working with a trained physical therapist is learning safe and effective techniques for moving your back that won't cause injury or unnecessary pain. A physical therapist can also help you target the source of your back pain in ways that you wouldn't be able to do on your own.
What's more, physical therapy can also help you improve your ability to exercise and do other activities with COPD. It can teach you how to exercise while managing your COPD symptoms and work with other physical limitations caused by COPD.
Get Medication For Your Pain
Sometimes, the best treatment for back pain is medication. This is especially true for serious back injuries and many types of chronic back pain.
What kind of medication you need depends on the type of back pain you experience and how frequent and severe it is. Here's a quick look at which medications work best for different types of back pain.
Drugs for Acute Back Pain
What kind of medication is appropriate for acute back pain depends mostly on how severe it is. Because acute pains tend to get better relatively quickly, you usually only have to take medication for a short time until your discomfort begins to improve.
If the acute back pain is only minor, then simple over-the-counter pain relievers should work well enough that no heavier drugs are needed. Medications like ibuprofen, Advil, Aleve, and topical creams can usually to do the trick.
If your pain is more severe or over-the-counter medications aren't effective, you should see your doctor to get an evaluation. If the cause is muscular, your doctor might prescribe muscle relaxants, which are very effective at relieving back muscle pain.
If you experience severe back pain, your doctor might prescribe you a heavier painkiller like an opiate. Although they can cause side effects and be highly addictive, they can be very effective for short periods to help you get through the worst of the pain.
Drugs for Chronic Back Pain
Unlike acute pain, chronic back pain is long-term and often difficult to manage. To treat chronic back pain effectively, you need to work with your doctor to come up with an individual pain management strategy.
What kinds of medications and treatments you get is determined by the cause and severity of your pain. Depending on your unique situation, you may receive any one of the medications that are prescribed for acute or inflammatory back pain, or a combination of medications.
Although it may seem strange, many doctors also prescribe antidepressants to help with chronic back pain. That's because antidepressants can change how your brain processes pain, helping to suppress and dampen chronic back pain.
Antidepressants can also help you cope with the psychological difficulties that come with living with chronic pain. They can also help you cope with anxiety and depression, which often accompany chronic diseases like COPD.
Drugs for Inflammation and Arthritis-related Back Pain

To start with, anti-inflammatory medications are often the first step to treating inflammation-related chronic pack pain. NSAIDs (Non-steroidal Anti-Inflammatory Drugs) are the most common type of drug prescribed, which include medications like Aspirin and Aleve.
Anti-inflammatory drugs relieve back pain by reducing inflammation in the bones and joints of your spine. It can also slow down the progression of arthritis by reducing the damage it does to your bones and joints.
Sometimes doctors prescribe drugs to suppress the immune system as a way to control severe inflammation. However, they prescribe these medications only sparingly because of their high risk for serious side effects like liver damage and anemia.
Doctors also prescribe other drugs like TNF-inhibitors and corticosteroids to treat arthritis-related back pain. But because they can have serious side effects, including infections and osteoporosis, doctors usually only prescribe corticosteroids for short periods of use.
The earlier you start treatment for inflammation and arthritis-related pain, the better your results will be. If you get diagnosed before the inflammation has caused too much damage, you may even be able to slow down or prevent some of the more advanced symptoms.
That's why it's important to talk to your doctor about your pain early and often, making sure to mention when anything changes or your pain becomes more severe. The more information you give your doctor, the more likely he is to be able to help you find a solution for your chronic back pain.
Treat Arthritis-Related Back Pain

As we mentioned before, people with COPD are prone to chronic inflammation and the myriad of other health conditions that chronic inflammation causes. This includes inflammation-related back pain and arthritis, including the spine-disfiguring condition ankylosing spondylitisis.
Aside from medication, there are certain habits and behaviors that can reduce inflammation-related back pain. Many of these include modifying your exercise routine to reduce spine strain and increase your back's movement and flexibility.
Tips for reducing inflammation-related back pain:
- Stay active to keep your spine flexible and strong.
- Stretch your back and other joints every day. Breathing exercises and back-extension exercises are often very helpful.
- Try light aerobic exercises that don't strain your spine, such as swimming or low-impact aerobics.
- Sleep with good posture on a firm mattress.
- Rearrange your living space to accommodate any movement limitations you have.
- Use chairs and furniture that support proper posture and support your spine when you sit.
- Don't smoke; tobacco smoking worsens inflammation and inflammation-related pains.
Other Therapies for Chronic Pain
So far, we've looked at a lot of different methods that you can use to specifically target back pain caused by COPD. However, there are also a variety of effective techniques for treating chronic pain in general that can be useful for treating chronic back pain.
These techniques can help relieve physical pain, muscle tension, and help you manage the psychological aspects of living with chronic pain. You can use them as an alternative or in combination with other pain medications and treatments.
Reduce Stress

Too much stress can do devastating things to your body and mind. It can cause physical pains, chronic inflammation (which can worsen physical pains), and cause serious mental disorders like depression.
As a result of these effects, chronic stress can both cause chronic back pain and make your back pain more severe. Over time, it can even rewire your brain to make it more sensitive to pain, amplifying any chronic pains you experience.
That's why, if you suffer from COPD, it's so important to look after your mental well-being and find healthy ways to manage stress. There are many ways to do this, including therapy, healthy lifestyle changes, and seeking support from family and friends.
To learn some helpful techniques for keeping stress under control, visit our guide on reducing stress and anxiety from COPD here. You'll find a plethora of practical methods you can use to relax, cope, minimize stress, and get rid of the major stressors in your life.
Get Psychological Therapy

Many people believe that there is nothing that psychological therapy can do for a physical issue like chronic back pain. The truth is, living with chronic pain can have serious effects on your mental health, and your mental health can also affect the severity of your chronic pain.
Many types of chronic pain, including back pain, have a psychological component. That doesn't mean that the pain is just in your head; it simply means that emotional and psychological distress can make chronic pains worse.
People with chronic pain are also more likely to experience stress, anxiety, and depression as a result of living in constant pain. Because of this, many people with chronic pains can more easily cope with their condition by seeing a psychological therapist.
Therapy can help you cope with your pain better, reduce your anxiety, and help you live a more fulfilling life. Treating your psychological symptoms may even be able to noticeably reduce the severity of your back pain.
Therapy can also help you deal with anxiety and mental distress caused by COPD. If you suffer from chronic pain and COPD, you should definitely consider seeing a therapist, especially if you also experience chronic anxiety, depression, or stress.
If you talk to your doctor, he may be able to recommend a good therapist or another mental health program for people with chronic pain or COPD. You can also find therapists in your area using online search tools like GoodTherapy or Find a Psychologist.
Try Mindfulness Meditation

This kind of meditation uses quiet reflection to help you calm both your body and mind. It can help you disrupt negative thought patterns about your pain and even change how your brain is wired so that you experience pain less intensely.
Research studies have proven that mindfulness meditation can be effective, if only slightly, for chronic pains. In addition, they show that it can also improve symptoms of depression, overall quality of life, and even emotional functioning in COPD patients.
Use Guided Imagery
This type of meditation helps you relax by focusing on positive thoughts and sensations. It can help you reduce stress, cope with your pain better, and serve as a distraction from your pain.
Studies show that guided imagery can be effective for pain caused by fibromyalgia and arthritis, and may even help psychological issues like anxiety and stress. This suggests that guided imagery could be effective for other chronic pains, including back pain caused by COPD.
Conclusion
Chronic back pain is difficult to live with, especially if you also suffer from COPD. It not only causes discomfort and limits your physical abilities, but it can significantly affect your overall quality of life as well.
Unfortunately, back pain can be a challenge to treat and often requires a multi-faceted treatment approach to manage effectively. That's why it's important to learn everything you can about how to treat and reduce back pain.
Through diet, exercise, healthy lifestyle changes, and psychological therapy, you can reduce or eliminate many different types of back pain. Whether it is acute, chronic, mechanical, or inflammatory, there are plenty of options you can try to get relief.
Everyone's body and experience with pain is different, so it may take some time before you find what works best for you. But you'll never know until you try, and with some trial and error you can figure out which treatment or combination of treatments is most effective for your pain.
That's why it's also important to talk to your doctor, especially if you suffer from chronic back pain. Your doctor can diagnose the source of your pain, point you toward the best options, and help you develop a long-term strategy for relief.


.png)





